Working in partnership to support clients with hepatitis during the pandemic
Steve says:
“At the beginning of the lockdown, we at the Hepatitis C Trust had to put our heads together to figure out new ways to engage with our clients. Normally, my job involves community outreach – engaging with people face-to-face – which of course just isn’t possible in a pandemic. That said, we still had patients to support, so while we were not able to hold our regular weekly clinics, we worked on other ways to ensure Hepatitis treatment could continue.
Alongside my work for The Hepatitis C Trust, I’m also a Peer Mentor for Forward, which means I’ve had a good insight into how drug and alcohol clients were being impacted by the lockdown. So once I, the environment I worked in and the clients I needed to support had been thoroughly risk assessed to ensure it was safe for us to interact, I made one of my priorities to team up with Forward and reach out service users who have Hepatitis C and use drugs like heroin. The lockdown had impacted the supply of street drugs, and I knew it could be clinically dangerous for them if they had to go through withdrawal very suddenly.
I worked with Forward to get these clients prescriptions for ‘opioid substitution therapy’ (OST) – basically legal medicines that have a similar effect on people as heroin, and are often used by doctors to help wean people off illicit substances. Forward were brilliant – they adapted to the situation fast to enable me to get patients sorted quickly.
My next project involved the ‘needle exchange’ service. Needle exchanges help users of intravenous drugs (such as heroin users) to safely dispose of used needles and obtain clean ones, in order to reduce the transmission of blood-borne infections like Hepatitis C.
I noticed that the number of people using the needle exchange service had dropped significantly during the lockdown, so I worked with Forward to deliver needle exchange supplies to service users, instead of them having to come to us.
I delivered supplies to the temporary homeless accommodation in Folkestone, which were then disseminated among the clients there. This worked really well and has now become an established part of the service. Harm reduction is a really important part of my role and I’m grateful to Forward, and in particular Forward’s Service Manager in Dover, Amelia, for providing me with the means to set this up.
As the lockdown began to ease, I was able to do a bit more face-to-face work, and I led on a project testing for Hepatitis C among homeless people who had been temporarily housed at the Travelodge in Canterbury. This was in conjunction with Porchlight, a local homeless charity, and the Rough Sleeping Initiative (RSI) Team, as well as Forward.
The testing went really well, so I approached Forward about screening other clients who had requested a test during the lockdown. Forward set aside a day at the Dover and Ashford hubs for testing and clients were invited to attend using a time slot appointment system so we could space people out and reduce the risk of large groups of people. I will be doing the same at Forward’s Margate hub soon, and possible in their Canterbury service as well.
Just before the lockdown, myself and two colleagues from Forward, Grace and Ian, did a three day testing event at Forward’s Dover & Folkestone Hub. The pandemic curtailed our normal follow up procedures, but I’ve now managed to start getting the process back on track and one client is due to start treatment soon, with hopefully more to follow.”
Grace says:
“We are working closely with The Hepatitis C Trust to deliver and plan testing for Hep C across East Kent. The Trust have been great, doing outreach with our clients even during these difficult times. It has been more important than ever that we encourage people to stay safe during the pandemic and we’ve continued to promote harm reduction through our needle exchanges as well as through interventions over the phone. We have exciting plans to improve and increase our testing for Hep C, so that we can reach all individuals across East Kent and ensure no one gets left behind”
The testing process
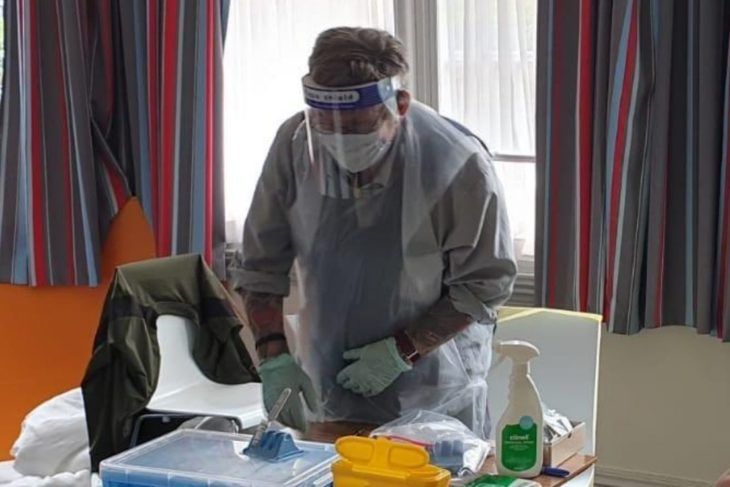
Hepatitis C Trust staff, including volunteers, wear full PPE at all times in the testing premises: masks and gloves, which are regularly changed, with hand sanitiser regularly applied. Those doing the testing are required to wear visors and aprons, which are also available to other staff members. The PPE is brought and taken away in clearly marked bags. There is also extra PPE for patients who get tested or anyone who displays or reports COVID-19 symptoms.
Clinicians test in a single, confidential area. Before starting testing, they wipe down surfaces in the room, and then test one patient at a time per tester. No one else other than the clinician and the individual being tested are in the room at any one time. Surfaces are wiped down after each patient and clinicians will either change or sanitise their gloves. Patients are expected to either wash or sanitise their hands in the sink or with the sanitiser provided before they enter the premises. They are also required to wear a mask that is supplied to them.
Before each test, clients are asked to give some information regarding themselves and their risk factors, including whether they’ve been tested before, and complete a consent form. Patients are brought in to be tested in order of forms completion, and their results are given to them privately afterwards. Everyone tested, regardless of their result gets a £5 voucher, to help incentivise participation.
People who test positive for the Hep C antibodies will require a further blood test to determine whether they currently have an active infection. If that is the case, blood forms are offered that they can take to the local hospital to get that done if willing or the team arrange to catch up with them post lockdown in conjunction with the hepatology nurse.